Damage to the brain can occur immediately, as a result of the injury, or it may develop from swelling or bleeding that can happen after the injury.
What happens when the brain is injured?
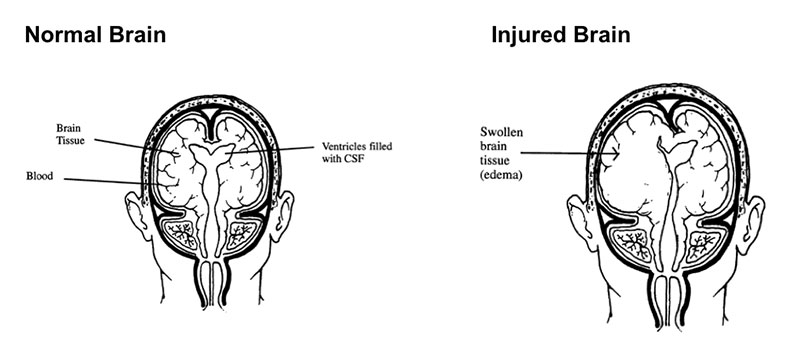
The skull is like a box that holds the brain, blood and CSF tightly together so that the brain doesn’t move around and get damaged during everyday activities.
After an injury, brain tissue may swell causing it to take up more room in the skull. This is called edema. When this occurs, the swollen brain tissue will push the other parts of the brain to the opposite side.
As the brain tissue swells or blood takes up space in the skull, the increase in pressurein the head rises and this can cause or be a sign of problems for the brain.
Increased pressure in the head interferes with the brain’s ability to carry out all of its important functions.
To understand this pressure, think of the skull as a hard box. After a brain injury, the skull may become overfilled with swollen brain tissue, blood or CSF. The skull will not stretch like skin to make room for the swelling brain. The skull may become too full and increase the pressure on the brain tissue. This is called intracranial pressure.
The doctors and nurses in the Intensive Care Unit (ICU) will be doing everything they can to try to keep the brain swelling down and prevent further damage from happening. Sometimes, even with all of the healthcare team’s efforts, the pressure will remain too high or the damage will be too bad that there may be little the team can do.
Intracranial pressure that is very high and does not come down even with treatment may be a sign of permanent brain damage and sometimes death.
Coma
When someone is in a coma they are unconscious. They do not speak and their eyes are closed. They may appear to be asleep, but they cannot be awakened. Sometimes patients in coma do not move at all, or they may have abnormal, very still body movements.
The length of coma varies from person to person. It can last from a few days to several months, or longer. Family members may expect a patient to suddenly wake up from a coma, but coming out of a coma is usually a very slow process. Usually, patients will become more aware of the people and things around them as they wake up from a coma. Predicting how quickly or how well a patient will come out of a coma depends on a number of factors such as the location, severity, and extent of damage. People may emerge from a coma with a combination of physical, intellectual, and psychological difficulties that need special attention. Some patients never progress beyond very basic responses, and some recover full awareness.
Family members and friends often wonder if comatose patients can hear. Sometimes patients seem to be calmed by a familiar voice or music. Since patients rarely remember these events later, it is impossible to know what they actually hear. Nevertheless, health care professionals recommend that people should speak to comatose patients as if they could hear and understand.
Patients in a coma can develop some medical problems because they are not moving on their own. Some of these problems include stiff joints, skin sores, infections and blood clots. The health care team will be working to try to prevent these problems from happening.
Minimally Conscious State
This is a term used for patients who are no longer in a coma. They may inconsistently follow simple commands and may have an awareness of their surroundings. They have reduced ability to respond and stay alert consistently during the day.
It is important not to provide too much stimulation (e.g. noise, touch, light) as the brain is not able to cope: this is gradually increased as the person makes progress.